Category: Health
-

Asian charity gets mayoral funding
•
The youth wing of Shakti Legal Advocacy and Family Social Services has secured a funding of $32,000 from the Auckland Mayoress’ Fund for Youth. The fund makes grants from money raised from the annual Westpac Mayoress’ Charity Gala Ball. The inaugural ball in November 2011 raised $170,000, and in its…
-
Outbreak of whooping cough gets worse
•
Health officials are urging Aucklanders to vaccinate their babies in light of the massive outbreak of whooping cough (Pertussis) in New Zealand’s largest city. There have been 322 cases of whooping cough reported in Auckland so far this year. This is five times higher than for the same time last…
-
Women feel unsafe in New Zealand – report
•
Many women are fearful about the crime culture in New Zealand, are tired of sex, and are resorting to desperate measures to succeed in life. These are just some of the findings of the 2012 NEXT Report, to be published in the next month’s issue of the NEXT magazine. The…
-

Early detection key to surviving bowel cancer – expert
•
Did you know that more people die because of bowel cancer than in road accidents in New Zealand? Bowel cancer is the second most common cancer and the second leading cause of cancer death in New Zealand. More than 1200 New Zealanders die from bowel cancer each year – one…
-

Why is junk food bad for you
•
The success of junk food business has drawn a lot of attention to the industry and the food itself. Many denounce junk food due to its ill effect on consumers and the health of the world. Not only is junk food confirmed to be bad for the physical condition owing…
-

Indian hospital provides remote care for rural areas
•
Nearly 70% of India’s population lives in rural areas, but 80% of its doctors are in urban areas. Rural patients often travel many kilometres for medical treatment. That is, if they can afford travel and cost of healthcare. Enter technology. In a small village -Â Chitradurga – in Karnataka, Â patients visiting…
-
Refugee doctor retires after 38 years
•
An Auckland doctor, known for his dedicated service to migrants and refugees, has set his stethoscope aside after 38 years of practice. Dr Nagalingam Rasalingam, 75, and his partner, Freddy Abeysekera have sold their Glen Innes practice, Line Road Medical Centre, to East Tamaki Health Care. The 6000-patient, very low cost access…
-

Flu shots safe for pregnant women – expert
•
As the winter approaches in Australia and New Zealand, health professionals are recommending flu shots for new and expectant mums. The safety of flu vaccination during pregnancy is well established and should be routine, according to the Royal Australian and New Zealand College of Obstetricians and Gynaecologists. The College says…
-

New Zealand to increase cigarette export to Australia
•
While fewer New Zealanders are smokers today than a decade ago, a cigarette manufacturer in New Zealand has attracted criticism for its plan to increase production of cigarettes for exports across the ditch. Imperial Tobacco’s Petone factory near New Zealand’s capital city of Wellington will quadruple its cigarette production with a two-year…
-
NZ women concerned about fertility
•
Two in three Kiwi women (63%) say they have friends and family who have experienced fertility issues and as many as 93% New Zealand women believe more should be done to promote ways to improve fertility. In response to an online survey by New Zealand’s Good Health magazine, the women said…
-
Campaign to get Asians to enroll for GP services
•
Members of Auckland’s Asian communities are being encouraged to enrol with a general practitioner (GP). A new public awareness campaign, Your Local Doctor, hopes to address lower than average enrolment rates among people of Asian descent in Auckland. Waitemata DHB epidemiologist Dr Lifeng Zhou says studies have consistently shown that…
-
Sleepy Canadian town gets relief for tortured women
•
When you come to Banff – a small, frozen town i the middle of 7000 sqkm Banff National Park, tourism is the first thing on your mind. It’s a sleepy town of just 7500 people in Canada’s western province of Alberta, caterig to a heavy inflow of keen skiers. Domestic…
-
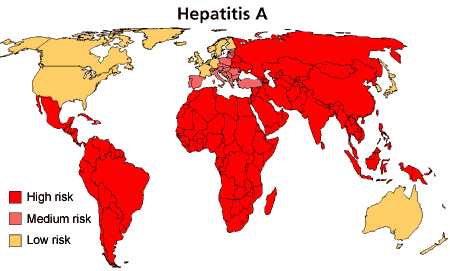
Hepatitis A outbreak: Auckland reports 31 cases
•
As many as 31  children have been diagnosed with Hepatitis A as public health officials warn that the number may increase. As these cases are affecting school age children,  the health officials are working with nine schools and affected parents to assess risk and provide advice. “This is an evolving…
-

Smoking bans in Australia coming soon
•
An upcoming smoking ban in Australia is prompting a New Zealand group to ask similar bans across the ditch. Under new sweeping changes introduced by Australia’s health minister, Jillian Skinner, diners in New South Wales will not be able to smoke in public dining places across the state. The new…
-
Meet the youngest person to get pacemaker
•
Fifteen minutes – that’s how old Jaya was when surgeons sliced open her chest to put pacemaker on her walnut-sized heart. A team of 20 medical staff attended to the 3-pound infant, soon after she was born with a heart beat of 45; a healthy new-born has a heart beat…
-

Mayor’s fund open for community grants
•
Money raised by the inaugural Auckland Mayoress’ Charity Gala Ball will soon be available to groups working with young Aucklanders as applications for grants are now open. The ball, hosted by Mayor Len Brown and Mayoress Shan Inglis last November, raised $170,000 towards the Mayoress’ Fund for Youth, an independent…
-
Teenagers face racism in New Zealand – study
•
Teenagers from ethnic and minority groups face many instances of discrimination based on race, a recent study has found. The survey of more than 9000 randomly selected secondary school students in New Zealand revealed that there were significant ethnic differences in the prevalence of ethnic discrimination. More than half of…
-

Internet may help cancer patients in recovery
•
Cancer patients face barriers to recovery in sparsely populated countries, and a researcher is looking to the internet to help build online support groups. A recently published research has identified barriers to physical activity for cancer patients which may slow their path to recovery. A New Zealand group has recently…
-

Orange juice ban in the US likely to cause other health issues
•
Temporary ban on the import of orange juices in the United States is likely to have a counter-productive effect, according to an industry expert. Parents worried about the fungicide may actually feed to their children more of it by switching to other juices, such as apple or grape juice, according…
-

India records a polio-free year
•
Thanks to a sustained eradication campaign, India has completed a year without recording a new case of Polio virus. India’s last reported case of the sometimes-fatal disease was a two-year-old girl in West Bengal State on 13 January 2011. The record seems even more remarkable against its historic figures –…